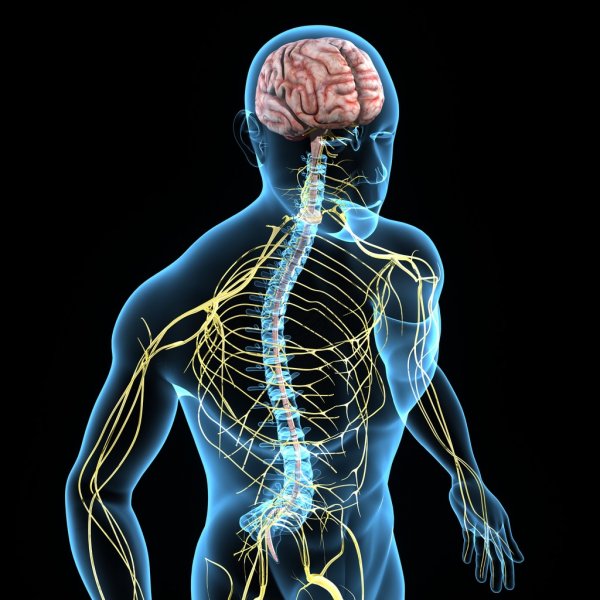
Function of the blood-brain barrier
The blood-brain barrier separates brain tissue from the circulation and plays an important role in protecting the brain from pathogens and toxins. Generally, only small, lipid-soluble molecules pass freely through it. However, the blood-brain barrier is impermeable to most macromolecules.1 Its barrier function is achieved through the formation of tight junctions between capillary endothelial cells in the brain. Notably, besides playing an important protective role, the blood-brain barrier also prevents many therapeutic candidates from entering the brain. Therefore, numerous strategies for drug delivery across the blood-brain barrier are being developed.
Strategies for drug delivery across the blood-brain barrier
Drugs can be delivered across the blood-brain barrier through approaches that either circumvent it or to disrupt it. Strategies that use blood-brain barrier disruption for therapeutic delivery include osmotic disruption, MRI-guided focused ultrasound, bradykinin administration, and radiation-induced disruption. Approaches that aim to circumvent the blood-brain barrier to deliver drugs include convection-enhanced delivery, viral-mediated circumvention, carrier molecules, liposomal delivery, polymer wafers, and P-gp targeting and modulation.2
Nanoparticles can be used as carrier molecules for drug delivery to the central nervous system. Magnetic nanoparticles can deliver drugs into the brain with the aid of magnetic fields, a process also referred to as magnetic drug targeting. Magnetic drug targeting requires the manufacturing of stable magnetic nanoparticles with good magnetic coupling and bioavailability. Moreover, it necessitates the design of an appropriate static magnetic field to drive the nanoparticles to the target.2 Magnetic nanoparticles contain a magnetic core that is stabilized by a protective biocompatible coating. Therapeutic agents or other functional groups can be attached to the magnetic nanoparticle. The nanoparticles can be administered systemically, and an externally applied magnetic field can facilitate their transport through the blood-brain barrier. Moreover, the magnetic heating that develops during this process increases the permeability of the blood-brain barrier.
Clinical applications of magnetic nanoparticles
Magnetic nanoparticles have already found applications in the clinical practice. They include their use as contrast-enhancing agents for magnetic resonance imaging, as magnetic vectors, for magnetic labeling and separation, and for magnetic hyperthermia and heating.
Magnetic nanoparticles for drug delivery across the blood-brain barrier
The technology for drug delivery with magnetic nanoparticles into the central nervous system is being actively developed. However, most studies are still limited to in vitro and animal in vivo models. The potential efficacy of magnetic nanoparticles as drug carriers is being investigated in models of glioblastoma, HIV central nervous system infections, Parkinson’s disease, and Alzheimer’s disease.3
Challenges in the development of magnetic nanoparticles for drug delivery into the central nervous system
The safety and toxicity of magnetic nanoparticles delivered in the central nervous system are being actively investigated with special focus on iron oxide nanoparticles.3 Moreover, technical challenges, including the diminishing magnetic field strength with target depth and poor retention after external magnetic field removal, are being assessed. Overall, magnetic nanoparticles hold great promise for the delivery of therapeutics across the blood-brain barrier, but technical and safety concerns should be addressed.